Insight’s ketamine clinic offers hope for Flint patients suffering from PTSD and depression
“I am happy. I feel good here.” Insight's ketamine clinic is providing much-needed relief to patients in Flint who suffer from post-traumatic stress disorder and depression.

The author of this Flinstide article is a registered nurse at IINN and provides care to patients in the ketamine clinic. The terms of this arrangement have been reviewed and approved by IINN and Flintside in accordance with its policy on objectivity. Some names, locations, and identifying characteristics have been changed to protect the privacy of those depicted.
FLINT, Michigan — At the age of twenty, Mike Foley was working as a patrol officer in one of the most violent, poverty-stricken cities in the country. Two decades later, he began to realize the cumulative toll the profession had on his mental health. He began to experience symptoms that left him feeling like his life was slowly being taken from him.
First responders and military personnel are trained to be watchful. They are constantly undergoing situational awareness assessments and are pushed to be hypervigilant. This continuous strain of stress, compounded with experiencing repeated traumatic experiences, can lead to the development of post-traumatic stress disorder (PTSD).
PTSD is a serious and often debilitating mental health condition that can arise after a person experiences a traumatic event. Symptoms of PTSD include flashbacks, avoidance triggers, negative changes in mood and cognition, and hyperarousal. Approximately 80% of patients with PTSD have at least one comorbid psychiatric disorder. The most common include depression, alcohol and drug abuse, and other anxiety disorders.
The average person sits with depressive symptoms for seven years before treatment is sought. It is the unseen physical damages that leave patients feeling continually worse, further negatively impacting an individual’s quality of life. Dr. Samantha Behbahani, a clinical psychopharmacologist, works with patients directly at Sanctuary Healthcare, a ketamine infusion clinic.
Behbahani is one of many clinicians turning towards the usage of ketamine for her patient’s care. In 2015, there were approximately 60 ketamine clinics. Today, there are more than 400 ketamine clinics in the United States.
“Patients will say to me when they’re depressed, ‘I feel like my brain is like molasses, like it just isn’t working.’ Well, if we look at an fMRI scan of a brain with depression, that’s what it looks like,” says Behbahani. “There’s not a lot of brain activity, not because the patient is not smart or intelligent. It’s that the neurons are not communicating quickly. We see neuronal atrophy and we’ll even see atrophy of the hippocampus.”
Ketamine functions at the NMDA receptors (N-methyl-D-aspartate) in the brain. It’s an antagonist at the receptor and allows for a surge of glutamate, an excitatory neurotransmitter. “This surge leads to a cascade of events, including neurogenesis, more neuronal growth, and synaptic strength,” says Behbahani. “Which is why patients will often say, [after receiving a ketamine treatment] ‘I feel like I can think more clearly, I feel like I have motivation to do things.’ We are allowing those neurotransmitters to speak to each other much faster.”
In the early 60s, Ketamine was first synthesized by Professor Calvin Lee Stevens’, PhD., team at Wayne State University. In 1964, ketamine was evaluated in a clinical trial and was quickly brought into use in clinical settings as a sedative for anesthesia. The low risk of respiratory depression quickly made ketamine a favored anesthetic. And when used as an anesthetic, its dissociative properties allow for pain relief and sedation.
Ketamine research for treatment-resistant depression began in the 1990s at Yale University. Depression has been historically understood as a serotonin neurotransmitter deficiency, but current research has revealed that the serotonin hypothesis only accounts for less than 20% of neurotransmitters in the brain. The other 80 percent of neurotransmitters in the brain are GABA and glutamate. Both of these transmitters create a push-and-pull response that sparks electrical activity in the brain. Further research into these two neurotransmitters revealed they may be responsible for regulating the majority of brain activity, including mood. During Yale’s study on ketamine, research revealed the medication triggers glutamate production, prompting the brain to develop neural connections.
Think of ketamine as falling snow and the brain as a sledding hill. After traumatic experiences, negative thinking patterns develop and sled routes are laid down the hill as semi-permanent paths. These routes, negative thinking patterns, are repeatedly ridden over and over, further impacting depression and stress. Ketamine allows fresh snow to be laid on the hill, allowing sleds to find new fresh paths.
At the University of Michigan, Dr. Sagar Parikh is a professor of psychiatry and has been using ketamine as part of his patient’s therapy for more than a decade. Parikh is also currently working on a research study to develop a blood test that would predict who will have a positive response to ketamine, by identifying biomarkers, specific enzymes within the body’s cells. “The ketamine is affecting this specific enzyme system and the people who show changes in the enzyme system, correlate to the patient’s improvement,” says Parikh.
In comparison to the VA hospital in Ann Arbor, U of M’s Ketamine clinic does not offer Ketamine therapy for PTSD as a primary diagnosis, but instead only offers it to patients with treatment-resistant depression. The VA does, however, not only offer ketamine as a treatment for PTSD but also covers the cost of IV ketamine therapy. Parikh’s rationale is, “The limited research that has been done shows that it is helpful as a treatment for depression, but research is limited in other areas. If someone has PTSD, that is not a disqualification, but they need to have a tough depression that’s not getting fixed. Many people with PTSD have low moods, but they’re not always suffering from severe depression.”
Parikh also identified contraindications for ketamine therapy that include any recent history of psychosis, active substance abuse problems, and history of recreational ketamine abuse. Another indicator that must be factored into ketamine IV therapy is if a patient is currently taking any medications that target GABA receptors and needs to be tapered off and discontinued. Medications that impact GABA receptors are Klonopin, Ativan, Xanax, and high doses of lamotrigine.
Dr. Evan Peskin, a triple board-certified anesthesiologist, is a physician currently working at Insight Institute of Neurosurgery & Neuroscience in Flint. Peskin has diligently worked with several combat veterans researching the effects of PTSD and the efficacy of ketamine as a means of treatment. IINN has recently developed a new Ketamine Infusion clinic under anesthesiologist Dr. Robert Maccani to expand care toward patients suffering from PTSD, treatment-resistant depression, and other chronic mental health issues.
“Unfortunately, getting help for PTSD can be frustrating,” says Peskin. “Many people with PTSD struggle to engage in traditional therapies, such as talk therapy, due to avoidance behaviors or difficulty or difficulty processing and expressing their thoughts and feelings. This can make it difficult for them to make progress in treatment and lead to feelings of hopelessness and frustration. One of the ways in which ketamine may be helpful for PTSD is that it can help to engage more fully in therapy. By reducing avoidance behaviors and increasing their ability to process and express their thoughts and feelings, ketamine can help people with PTSD make considerable progress in treatment.”
Behbahani, Peskin, and Parikh unanimously agree that patients who have gone into remission after their ketamine IV therapy will need maintenance doses in the future and ongoing psychotherapy. For each patient, the number of maintenance doses can range from a single infusion once a year or once a month, pending individualistic patient care that is closely monitored by a psychiatrist.
Foley, now in an administrative supervisor role with the police department, responded to a follow-up call that concerned a child who had just experienced life-endangering physical abuse. After securing the house, Foley was standing alongside one of his peers, facing the culprit responsible for endangering the child’s life. Suddenly, there was a shift. Something began to creep its way to the surface inside of Foley. He started to burn with heat and sweat. His stomach a knotted mess, Foley began to imagine the pleasure he would feel if he could just lash out and create an impact on the culprit. Foley knew he had to get out of the home fast.
“I looked over at the other fella that worked with me in the department, and I said, ‘I have to leave right now. I have to leave or I am going to get myself into trouble. I just walked the f*ck out and left. I was just angry as f*ck. I f*cking hate when people are victimized who are not able to defend themselves,” says Foley. He could see the clues within himself that his bottling up of memories and stress was creating a chronic amount of pressure and tension within his own body. Foley was beginning to show signs of cumulative post-traumatic stress disorder.
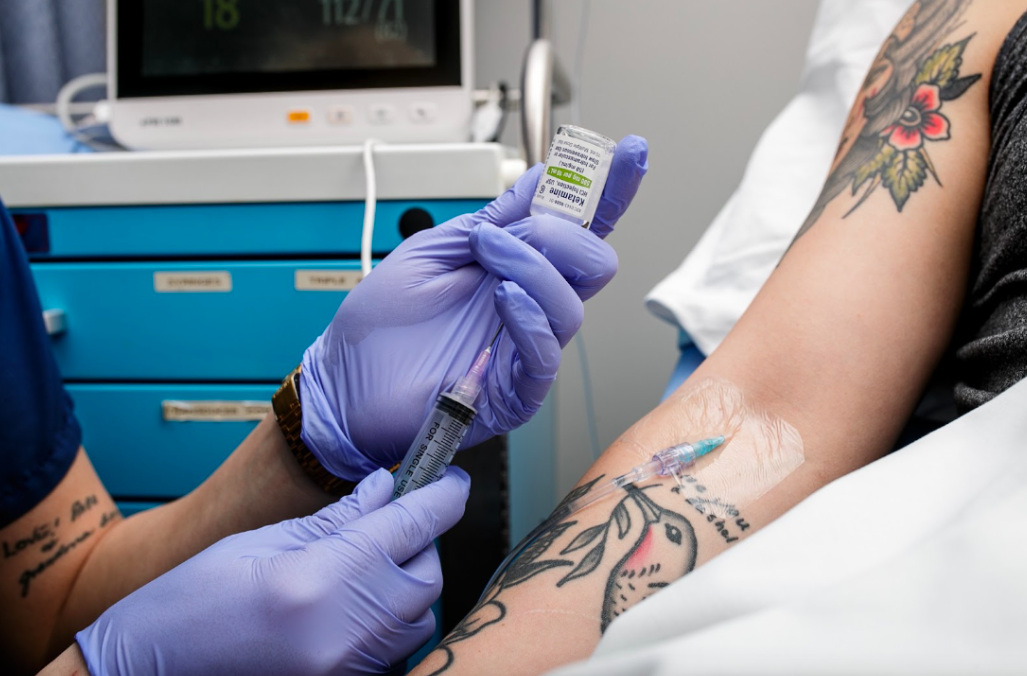
He continued working as an officer and ignored the first clues that PTSD was grabbing a hold of his life. He would notice a week would go by and he had drank alcohol every single day after work. Foley would attempt to slow down his drinking, but a few weeks would go by and he would be back to drinking heavily again. Foley’s anger, drinking, and withdrawal began to catch his wife’s attention.
“I mean, very openly, my bride says to me after a trip out of town, ‘You know, you need to go talk to somebody’,” says Foley. “I had moments that I had shared with her, but like lots of us that have been stressed out or pushed to the max, you say all these things, but you never follow through.”
A true lover of stories, Foley began reading and listening to anything he could get his hands on that told of men and women who were combat veterans and survivors, while he started psychotherapy. He found a recurring theme: several of these survivors with PTSD had undergone psychedelic treatments.
“I’ve heard it over and over with these guys. These experiences are completely life-changing and gave them their f*cking lives back,” Foley says. “And I mean, I was the guy saying, ‘I am buying a f*cking plane ticket, and I am gonna go lick some frog somewhere and I am gonna be going f*cking bananas in the jungle, but I don’t give a f*ck. I f*cking need help.”
There was finally a chance for hope for Foley, a chance to get his life back. He found a local ketamine clinic at Insight.
“I was nervous, I was scared, but I was so f*cking excited at the same time, at the chance for hope. I just didn’t want to feel like sh*t anymore,” says Foley.
Foley underwent six ketamine infusions at IINN over a two-week period, each infusion lasting approximately an hour. “I remember feeling this almost intoxicating effect of ‘I’m not in control anymore of myself. I gotta just let go and ride this f*cking wave.’ There was so much going on in my mind at a speed I could not even f*cking comprehend. It felt like being on the front of a rocket. I felt I was everything and nothing all at once.”
On the following day after his first infusion, Foley went to a trampoline park with his children for a birthday party. Normally, a public place filled with people would have triggered his PTSD. He would be constantly assessing who and what could bring about the most danger in the room and ultimately be unable to be completely present. This time, it was different.
Tears started to roll down Foley’s face. His wife walked over, reached out, and asked what was wrong. Overwhelmed with emotion, being able to participate and be engaged, Foley couldn’t believe it. The funk, the cloud, they were finally lifting.
“I’m crying because I am so f*cking happy that I am having fun with my kids,” said Foley. “I am happy. I feel good here.”






